INTRODUCTION
Syphilis is an infectious disease transmitted mainly through sexual intercourse and that can have several presentations at various stages [1]. Tertiary syphilis, now rare due to effective antibiotic treatment already in use for several years, is responsible for cardiovascular syphilitic lesions [2,3]. Among the lesions, the most common is the syphilitic aortitis. In untreated syphilis, aortitis may manifest after 10 to 40 years after the initial sexual contact [2,3]. The ascending aorta is affected in 50% of the cases, followed, in descending order, the aortic arch, the descending aorta and abdominal aorta, with possible impairment of coronary ostia and aortic valve [2,4].
The main cause of death occurred in about 80% of cases, and rupture of saccular aneurysms, when not treated surgically [4].
After primary infection, there is the presence of
Treponema pallidum in the aortic wall, initially in the adventitia and soon after in the lymphatic vessels. This is one of the main reasons for the tropism of spirochetes in relation to the ascending aorta, since it is rich in lymphatics [2,4].
The
vasa vasorum undergoes a process of endarteritis obliterans, necrosis of medial layer (mesoarteritis), and infiltration of plasma cells. Consequently, the elastic tissue of the vessel is destroyed and replaced by scar tissue. The inflammatory process may continue for a long time and can be found until 25 years after initial infection [2,5].
The clinical presentation may be of angina when there is obstruction of the coronary ostia, dyspnea, when there is aortic failure. However, the most common clinical symptom is chest pain secondary to rapid expansion of the luetic aneurysm [2].
CASE REPORT
48-year-male patient, brown. His main complaint was "shortness of breath". The patient reported that he noticed dyspnea on efforts for one year. He did not undergo follow-up. Dyspnea was increasing steadily and currently had dyspnea on moderate effort, accompanied by non-characteristic chest pain. This pain has drawn attention from family members, who opted for medical advice. History of promiscuity, with a case of gonorrhea of difficult treatment for 30 years. He denies family heart disease or other comorbidities, without using drugs.
On physical examination, the patient was in good condition. Normal colored, hydrated, eupneic, acyanotic and anicteric. Blood pressure was 160x80 mmHg. Peripheral pulses in water hammer. Without edema.
On cardiac auscultation presented holodiastolic blow in all outbreaks, predominantly in the aortic area. Lungs were clear. No other significant changes on physical examination.
On chest X-ray presented increased heart size and aortic ectasia. The electrocardiogram showed sinus rhythm, without significant changes. Doppler echocardiography revealed evidence of enlargement of the aortic root (47 mm diameter), significant increase in left ventricular ejection fraction of 55%. Aortic valve with significant regurgitation.
Cardiac catheterization showed normal coronary circulation, increased left ventricular end systolic volume due to diffuse hypokinesia +++/++++. Aortography revealed aortic caliber and aortic valve with severe regurgitation (Figure 1).

Fig. 1 - Aortography showing enlargement of the ascending aorta and reflux of contrast to the left ventricle, demonstrating the aortic failure
Surgical approach was performed through median thoracotomy, cannulation of the aorta, superior and inferior vena cava. Cardiopulmonary bypass (CPB), clamping of the ascending aorta, cardioplegic solution infused into the coronary ostia were initiated. The incision was performed earlier in the ascending aorta with visualization of the failed aortic valve and the ascending aortic wall with calcification and signs of degeneration. The patient then underwent aortic root reconstruction with implantation of a valved Dacron tube 25 (Figures 2 and 3). Total CPB time was of 100 minutes. The surgery was uneventful.
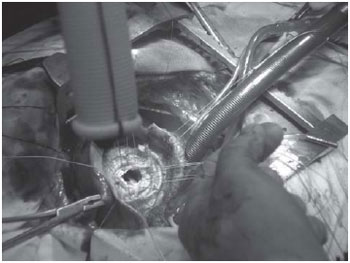
Fig. 2 - Surgical field at the time of insertion of the Dacron tube. Visualization of the aortic valve and tube

Fig. 3 - Dacron tube positioned between the aortic root and its proximal third
Postoperatively, the patient developed symptomatic anemia (weakness), requiring infusion of two units of pRBCs.
Due to the degenerative appearance of the aortic root, diagnostic tests for syphilis were then requested. The result of VDRL, 1:32, and FTA-ABS-IgG antibody reagent. Anti-HIV negative.
The aorta was submitted to histopathologic study (Fig. 4), which returned the following report: adventitia showing foci of cellular infiltrate with lymphocyte predominance;
vasa vasorum with signs of thickening of the intima, tunica media with signs of focal ischemia, small areas of necrosis, plasma cell infiltration; intima with atherosclerotic plaques.

Fig. 4 - Surgical piece (thoracic aorta), showing rugose appearance, yellowish, with small thickening, suggesting the degenerative presentation of the aortic root
Patient recovered uneventfully and was discharged nine days after surgery, with the treatment regimen for syphilis tertiary.
On postoperative follow-up, the patient progressed uneventfully, with regular clinical follow-up.
DISCUSSION
The basic lesion of cardiovascular syphilis is aortitis. Myocarditis and myocardial syphilitic gums are rare. There is, not infrequently, an association of this lesion with coronary heart disease due to the presence of contiguity [2]. The case described showed no such association, confirmed by cardiac catheterization and during surgery, although the chest pain reported by patients.
Valvular involvement in the case described is due to enlargement to the aortic annulus followed by dilation of the aorta. There is often a direct involvement to the valves by the disease, but due to a condition of severe regurgitation was necessary to replace it.
The patient presented heart failure due to the presence of chronic aortic regurgitation untreated. No syphilitic myocardial lesions were found.
There is the availability of more sensitive laboratory tests (such as computed tomography), which are of choice in cases of aortic lesions [2], but the echocardiogram and cardiac catheterization were enough to define the lesion with sufficient accuracy, for surgery.
During the surgery, immediately after thoracotomy, it was observed that the aortic root had a rough exterior and yellow coloring. At the touch, the aorta was hardened and presented irregularities. It was then suggested the diagnosis described.
Other diagnoses were considered - the giant cell arteritis (or temporal arteritis) and Takayasu's arteritis - due to the involvement of the aorta by both diseases. Despite the giant cell arteritis involves large-caliber arteries, such as temporal, carotid and vertebral arteries and aorta, it most commonly affects the elderly. However, the Takayasu's arteritis, which also involves large arteries, mainly through stenotic inflammatory lesions of the aorta and its primary branches, most commonly affects young women [6]. Both diseases were excluded due to clinical and serological confirmation of the underlying disease of the patient.
In previous reports, it is used the femoral cannulation for CPB, due to the large inflammatory process in the ascending aorta. We opted for aortic cannulation in the transition between the ascending aorta and aortic arch because the inflammatory process is restricted to the aortic root.
The postoperative treatment with benzathine penicillin, in doses recommended for tertiary syphilis, is regularly implemented to decrease the chances of relapse. However, it is known that even with the elimination of
Treponema Pallidum in the system, the chance of recurrence of the disease still persists [3]. Because of this, there is a need for a long-term follow-up of the patient.
Syphilitic aortitis is a manifestation of acquired syphilis, not occurring in congenital syphilis. Currently, the manifestations of tertiary syphilis are less common due to the advent of penicillin therapy [2]. But we must consider that there is a direct relationship with the patient's socioeconomic conditions and development of disease.
Treatment of severe syphilitic aortitis is surgery. The diagnosis of syphilitic aortitis is not currently contemplated by the rarity of the case, because the current treatment with antibiotics is largely complete and, if treated properly, is extremely effective. In this case, the surgeon's experience was capital to the diagnosis, since it was not considered the hypothesis before the observation of the aortic lesion. In Brazil, we still have important socio-cultural conflicts, reflecting the social health - leading syphilis as a possible diagnosis.
1. Machado MN, Trindade PF, Miranda RC, Maia LN. Lesão bilateral dos óstios coronários na sífilis cardiovascular: relato de caso. Rev Bras Cir Cardiovasc. 2008;23(1):129-31. [MedLine] View article
2. Corso RB, Kraychete N, Nardeli S, Moitinho R, Ouvires C, Barbosa PJ, et al. Aneurisma luético de arco aórtico roto, complicado pela oclusão de vasos braquiocefálicos e acidente vascular encefálico isquêmico: relato de caso tratado cirurgicamente. Rev Bras Cir Cardiovasc. 2002;17(2):63-9. View article
3. Avelleira JCR, Bottino G. Sífilis: diagnóstico, tratamento e controle. An Bras Dermatol. 2006;81(2):111-26.
4. Carrada-Bravo T. Sífilis cardiovascular: diagnóstico y tratamiento. Arch Cardio Mex. 2006;76 Supl(4):189-96.
5. Mattos AD. Sífilis cardiovascular. An Bras Dermat. 1970;45:267.
6. Cruz BA. Arterite de Takayasu e arterite temporal (arterite de células gigantes). Rev Bras Reumatol. 2008;48(2):106-9.




 All scientific articles published at www.rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at www.rbccv.org.br are licensed under a Creative Commons license