OBJECTIVE: To comparatively analyze minimally invasive procurement of saphenous veins using Mini-Harvest® system and a technique using adapted traditional instruments.
METHOD: From June 1996 to January 1999, 63 patients who were submitted to Coronary Artery Bypass Grafting Surgery had their saphenous veins resected using minimally invasive techniques. In the first 30 patients of the series, a direct visualization method employing two Langenbeck's retractors was utilized and for the 33 remaining patients the Mini-Harvest® technique was utilized.
RESULTS: The mean age of the patients was 61 ± 8.75 years old. Fifty-two patients were male and 11 female. Forty-five patients were diabetics, 45 were overweight or obese, 25 were smokers and 32 presented history of myocardial infarction. The mean time to resect the saphenous vein using the Langenbeck's retractors was 34.2 ± 8.14 minutes and using the Mini-Harvest® it was 39.20 ± 9.12 minutes. The lenghts of the extracted veins were similar in both groups, varying between 10 and 30 cm. There was one case of superficial dehiscence in the Langenbeck group. With two patients in the Mini-Harvest® group and one in Langenbeck's group it was necessary to revert to the traditional method of procurement. The incidence of tran-soperative infarction was 4.5% (three patients) in Langenbeck's group and 3.1% (two patients) in the Mini-Harvest® group.
CONCLUSIONS: We can conclude that the minimally invasive procurement methods of the saphenous vein by direct visualization are effective and safe, both when employing adapted traditional instruments and using purpose-made retractors. We stress, however, that the Mini-Harvest® method does not require an assistant.
OBJETIVO: Analisar, comparativamente, a obtenção minimamente invasiva com o uso do MINI-HARVEST® e com instrumental tradicional adaptado.
MÉTODO: De junho de 1996 a janeiro de 1999, 63 pacientes submetidos à cirurgia de revascularização do miocárdio tiveram suas veias safenas retiradas segundo técnica minimamente invasiva. Nos 30 primeiros pacientes da série utilizou-se método de visão direta com auxílio de dois afastadores de Langenbeck, e nos 33 restantes utilizou-se o MINI-HARVEST®.
RESULTADOS: A idade média dos pacientes era de 61 ± 8,75 anos, sendo 52 homens e 11 mulheres. Quarenta e cinco pacientes eram diabéticos, 45 apresentavam sobrepeso/obesidade, 25 eram tabagistas ativos, 32 apresentavam história pregressa de infarto do miocárdio. O tempo médio de retirada da veia safena com afastadores Langenbeck foi de 34,2 ± 8,14 minutos e com o MINI-HARVEST® de 39,20 ± 9,12 minutos. A extensão de veia retirada foi similar nos dois grupos, variando de 10 a 30 cm. Houve uma deiscência superficial no grupo com afastadores de Langenbeck. Houve necessidade de reversão para método tradicional de retirada em dois casos do grupo MINI-HARVEST® e um do grupo Langenbeck. A incidência de infarto transoperatório foi 4,5% (três) no grupo Langenbeck e 3,1%(dois) no grupo MINI-HARVEST®.
CONCLUSÕES: Podemos concluir que o método de obtenção de veia safena minimamente invasivo sob visão direta é efetivo e seguro, tanto com o uso de instrumentos tradicionais adaptados para este fim, como com afastadores especialmente constituídos, ressaltando-se que o MINI-HARVEST® dispensa a presença de um auxiliar.
INTRODUCTION
Minimally invasive surgeries are characterized by reduced surgical trauma and they are associated with smaller incisions. Both direct visualization and endoscopy can be employed [1]. General thoracic surgery has also benefited from minimally invasive methods [2]. In heart surgery, coronary artery bypass grafting is of great importance, both without the use of cardiopulmonary bypass or with reduced incisions. The saphenous vein is still a commonly utilized graft [3]; thus, minimally invasive methods for its procurement are desirable, as these techniques reduce surgical trauma and result in better esthetic results. The methods that utilize a totally endoscopy technique present advantages, as they only require one or two small incisions, allowing the removal of long segments of saphenous veins [4]. The disadvantages of these methods are the cost and the space used for the surgery that can delay the opening of the thorax. Methods of procurement under direct visualization can be as simple as the approach used by STAVRIDIS [5] or more refined with the use of special retractors [6].
Our aim was to compare procurement of saphenous veins by the minimally invasive method, under direct visualization and with the use of adapted retractors (Langenbeck) or with purpose-made retractors for this procedure (MINI-HARVEST ® - USSC-Cardiothoracic System, Newalk).
METHOD
From June 1996 to January 1999, 63 patients submitted to their first elective surgery of coronary bypass grafting had saphenous veins resected by a minimally invasive method under direct visualization. The first 30 patients of the series (Group1) utilized a method using two Langenbeck retractors. The remaining 33 patients (Group 2) underwent surgery using a method with MINI-HARVEST ® retractors that are specifically made for this procedure. The patients were evaluated in respect to age, gender, smoking, weight (overweight or obese), previous infarction, diabetes, time to remove the vein, necessity to revert to traditional resection method, infection and dehiscence at the suture, trans-operative infarction and death.
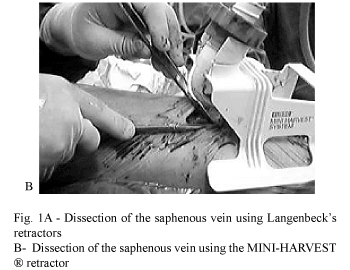
In the Group 1, using Langenbeck retractors and a light source, the incision was initiated near to the inguinal fold and the saphenous vein was dissected and isolated. A subcutaneous tunnel approximately 1/3 of the thigh was performed, where a new incision of approximately 3-4 cm was made. After dissection of this segment of vein, a new tunnel was created to near to the knee and so on successively until the length of vein was sufficient for the surgery. With the help of one assistant, the Langenbeck's retractors were positioned so as to enable visualization of the subcutaneous venous path (Figure 1A)
The branches were tied with LT 100Ethicon ligaclips ®.
In Group 2 the same method was used with the exception that no surgical assistant was necessary. (Figure 1 B).
The traditional method was used for the thoracic stage of the surgeries, that is, median sternotomy with cardiopulmonary bypass using crystalloid or sanguineous cardioplegic solutions. Anastomosis of the left internal mammary arteries to the anterior interventricular artery was utilized in under 70-year-old patients. Patients were considered diabetics if their disease had previously been diagnosed and they were being treated, using oral hypoglycemic agents or insulin. Active smokers were all patients who continued to smoke during the month leading up to surgery. Overweight/obese patients were all the patients with at least 20% over the ideal weight for their age. Trans-operative infarction was considered if a new Q-wave appeared and or if there was an accentuated reduction in the R-wave. In this study hospital mortality was recorded. This study was assessed and approved by the Local Committee on Ethics in Research.
RESULTS
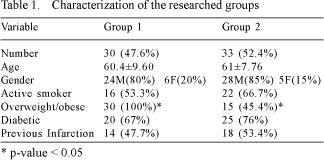
Table 1 summarizes the results referring to the participants of the two groups.
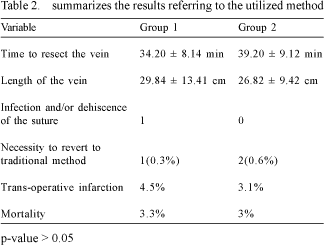
Table 2 summarizes the results referring to the utilized method.
COMMENTS
When comparing the two groups there was only a significant difference in the diabetes. (according to presented facts on list 1, the groups were distinct only if overweight/obese and not if diabetic). This might be explained by the fact that the patients were not randomly allocated to the two groups. Thus, at the beginning of our study, we used the minimally invasive method in diabetic and obese patients, that is, in those patients with a higher risk of evolving with infection or dehiscence of sutures.
With the increased experience and the use of the MINI-HARVEST® we started to utilize the method considering the esthetic results too, but even then always indicating patients with higher risks of complications. This can explain the greater number of overweight and diabetic patients when compared to the literature [7,8].
There were no significant differences between both methods in relation to the resection time of the saphenous vein. Even though no comparison was made, the time required by both these methods for saphenous vein procurement is greater than the traditional method, but there has been an improvement with experience. The mean time we obtained is in accordance with the literature [5,6]. The lengths of the extracted saphenous veins were similar in the two groups, compatible with an average of 2.5 grafts in each group. There was no difference in respect to the necessity to revert to the traditional method. The presence of an assistant in the Group 1 facilitated the approach, but the second generation of MINI-HARVEST®, enables excellent access to the vein inside of the subcutaneous tunnel. The greatest concern with the new methods is related to the integrity of the grafts, particularly to its endothelium. Some authors have evaluated its integrity using endoscopic methods and retractors similar to the MINI-HARVEST® and they concluded that these methods enable the resection of saphenous vein grafts with preservation of the endothelium [9,10]. We did not perform this type of analysis but based our assessment only on the incidence of trans-operative infarction and mortality; several factors are involved with this variable, such as the anastomosis technique, the distal coronary bed, the method of myocardial protection and the ventricular function. However, it is incontestable that a badly preserved or injured graft during resection is associated with a higher incidence of occlusion [11]. In this series we had one death in each group. In Group 1, the death occurred due to a brain stroke and in Group 2, due to low output syndrome in the postoperative period. There were no significant differences between the two groups in respect to these variables, with the values in harmony with those reported in the literature for coronary artery bypass grafting surgery using cardiopulmonary bypass and cardioplegic protection [12].
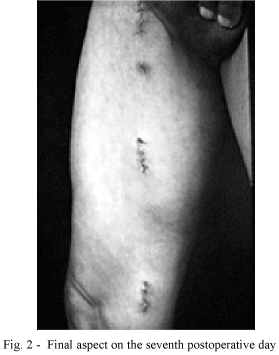
We did not find significant differences in respect to the incidence of infection or dehiscence of sutures. There was only a superficial dehiscence in Group 1. Some authors [13-15] analyzed the presence of hematomas, edema and pain. We preferred not to do this, as these criteria are too subjective. Obviously the esthetic aspect is incontestable, the best results seen with minimally invasive methods (Figure 2). The degree of esthetic expectations varies from patient to patient and with their economic and social levels. We did not find any scoring system in the literature applicable to our population.
CONCLUSIONS
The minimally invasive method of saphenous vein procurement under direct visualization is as effective and safe both using traditional instruments adapted for this purpose and with retractors specifically manufactured for the purpose. The only advantage of the MINI-HARVEST® system is that it does not need the presence of an assistant.
BIBLIOGRAPHIC REFERENCES
1 Morris RJ, Buttler MT, Samuels LE. Minimally invasive saphenous vein harvesting. Ann Thorac Surg 1998;66:1026-8.
[ Medline ]
2 Demmy TL, Curtis JJ. Minimally invasive lobectomy directed toward frail and high-risk patients: a case-control study. Ann Thorac Surg 1999;68:194-200.
[ Medline ]
3 Dias RR, Jatene FB, Jatene AD. Dissecção minimamente invasiva da veia safena para obtenção de enxerto venoso na cirurgia de revascularização do miocárdio. Rev Bras Cir Cardiovasc 1997;12:244-7.
[ Lilacs ] [ SciELO ]
4 Allen KB, Shaar CJ. Endoscopic saphenous vein harvesting. Ann Thorac Surg 1997;64:265-6.
[ Medline ]
5 Stavridis GT, Bobos D, Matsouka F, Lacoumenta S, Alivizatos PA. Minimally invasive long saphenous vein harvesting using a laryngoscope. Heart Surg Forum 1998;1:37-40.
6 Yeh CH, Chang CH, Lin PJ, Tsai FC, Yang MW, Tan PP. Totally minimally invasive cardiac surgery for coronary artery disease. Eur J Cardiothorac Surg 1998;14(Suppl 1):S-43-7.
7 Parsonnet V, Dean D, Bernstein AD. A method of uniform stratification of risk for evaluating the results of surgery in acquired adult heart disease. Circulation 1989;79:I3-12.
[ Medline ]
8 Paniágua PR, Rezende MC, Carranza RB, Gomes CRM, Sabatovicz Jr. N, Marques DLL et al. Cirurgia de revascularização do miocárdio com enxertos compostos. Rev Bras Cir Cardiovasc 1999;14:14-8.
[ Lilacs ] [ SciELO ]
9 Cable DG, Dearani JA, Pfeifer EA, Daly RC, Schaff HV. Minimally invasive saphenous vein harvesting: endothelial integrity and early clinical results. Ann Thorac Surg 1998;66:139-43.
[ Medline ]
10 O`Regan DJ, Borland JA, Chester AH, Pennell DJ, Yacoub M, Pepper JR. Assessment of human long saphenous vein function with minimally invasive harvesting with the Mayo stripper. Eur J Cardiothorac Surg 1997;12:428-35.
[ Medline ]
11 Roubos N, Rosenfeldt FL, Richards SM, Conyers RA, Davis BB. Improved preservation of saphenous vein grafts by the use of glyceryl trinitrate-verapamil solution during harvesting. Circulation 1995;92(9 suppl):II31-6.
12 Grover FL. The Society of Thoracic Surgeons National Database: current status and future directions. Ann Thorac Surg 1999;68:367-76.
[ Medline ]
13 Tran HM, Paterson HS, Meldrum-Hanna W, Chard RB. Tunnelling versus open harvest technique in obtaining venous conduits for coronary bypass surgery. Eur J Cardiothorac Surg 1998;14:602-6.
[ Medline ]
14 Tyszka AL, Fucuda LS , Tormena LB, Campos ACL. Obtenção da veia safena magna através de acesso minimamente invasivo para revascularizações miocárdicas. Rev Bras Cir Cardiovasc 2001;16:105-13.
[ Lilacs ] [ SciELO ]
15 Black EA, Campbell RK, Channon KM, Ratnatunga C, Pillai R. Minimally invasive vein harvesting significantly reduces pain and wound morbidity. Eur J Cardiothorac Surg 2002;22:381-6.
[ Medline ]
 All scientific articles published at www.rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at www.rbccv.org.br are licensed under a Creative Commons license